Vitamin D receptor, a powerful weapon against colorectal cancer
Vitamin D receptor, a powerful weapon against colorectal cancer
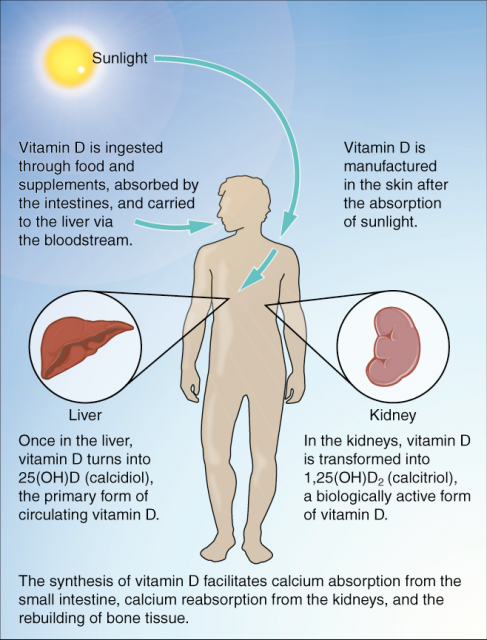
Vitamin D is an atypical vitamin because it is not a real vitamin. Vitamins are supposed to be essential, meaning that our organism cannot live without them but their synthesis cannot take place in our cells, so we must ensure an external intake through the diet. However, only 10% of vitamin D daily requirements come from the diet, and 90% is photochemically produced in our skin on the presence of UVB radiation, that is, sunlight.

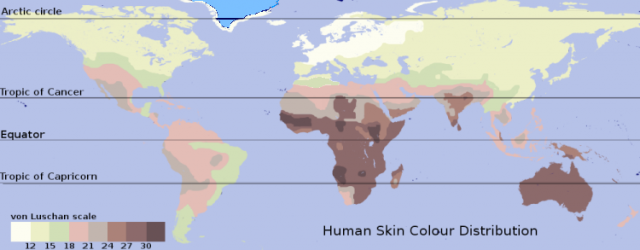
Hence, our body requires sun exposure to synthesize vitamin D. Recommendations about the time of sun exposure needed to cover vitamin D daily requests are vague as these depend on the energy of sun radiation, which ultimately depends on latitude (distance from the equator) and season of the year. Moreover, each of us synthesizes and regulates vitamin D levels differently in accordance to age (it decreases as we grow older), skin colour (there are lower levels in dark skin), metabolism, weight…
Tentatively, someone who lives in Spain and is commonly healthy will have enough with a 15-30 minute walk twice a week (April to October) to produce the vitamin D he or she needs. In winter, however, the energy received from the sun in the Spanish territory is quite lower, so we must increase vitamin D dietary intake or otherwise our vitamin levels will drastically decrease. Vitamin D has an evolutionary significance in Homo sapiens skin pigmentation: it is responsible for the loss of pigmentation and skin colour distribution around the world (skin is lighter in higher latitudes, where insolation is lower). But this is such an interesting story that it deserves its own post.
At this point, there are two issues that should be clarified: firstly, beneficial effects of sunlight (due to vitamin D synthesis) cannot be an excuse for uncontrolled sun exposure. On the contrary: excessive exposure to sunlight raises the risk for skin cancer. For that purpose, dermatologists and many other experts recommend protecting skin from too much sun exposure or, more practically, limit time exposure. Secondly, it is critical to seek medical advice before taking vitamin D supplements. Not only because it is imperative to know about the vitamin status of the organism before following a medical treatment, but also because an excess of vitamin D may damage your health and aggravate certain pathologies (renal insufficiency, granulomatous diseases, and so on).
In the diet, the main sources of vitamin D are oily fish (or blue fish): salmon, tuna, anchovy, herring and mackerel. There are other vitamin D rich foods, although in this case vitamin levels are lower.
The multiple effects of vitamin D on the organism are not exerted by the molecule itself but by some of its derivatives, especially calcitriol (technically, 1,25-dihydroxyvitamin D3). Calcitriol is generated in the kidney and other tissues and is considered a key hormone for calcium and phosphate regulation and, accordingly, for bone biology. It also participates in the regulation of the immune system and in the control of proliferation and survival of different cell types. These regulatory effects on the cell cycle connect calcitriol to cancer.
Many epidemiological studies show that vitamin D deficiency is associated with an increased risk of cancer, particularly colorectal cancer, a major cause of mortality worldwide (around 40,000 new cases are diagnosed every year Spain).
At the molecular level, calcitriol action is mediated by a receptor that is preferentially located in the nucleus of the cells (vitamin D receptor or VDR). VDR exerts its role in two ways: it binds to DNA controlling the transcription of many genes and it operates in other metabolic pathways. In fact, the calcitriol-VDR bond is a key regulator of the human genome, as it modulates the expression of more than a thousand genes.
Human colon epithelial cells express VDR as well as many of the colon tumour cells, so it has been suggested that VDR detection may be lead to improve medical diagnosis. On the other hand, it has been experimentally tested that calcitriol modifies gene expression in colorectal cancer cells, diminishing its proliferation and malignancy. The findings accomplished by Dr. Muñoz’s group have significantly contributed to establish this connection.
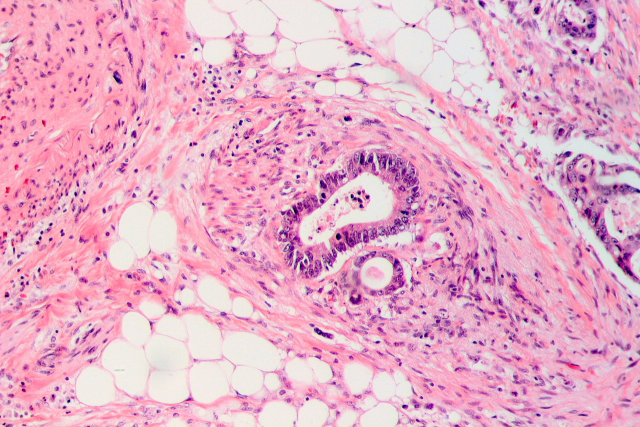
Currently, Dr. Muñoz’s lab focuses on detecting which genes and proteins are regulated by calcitriol in human colorectal cancer, both in tumour cells and in other cells that enclose the tumour (fibroblasts mainly), which are part of the so-called tumour stroma. They also study the effect of calcitriol on stem cells, as alterations on their physiology have been proposed to be a cause for cancer initiation.
Dr. Muñoz’s group studied 1 the expression of VDR and two VDR-controlled genes in 658 colorectal cancer patients. This work reports the role of tumour stroma fibroblasts on cancer development. The results derived from these experiments associate VDR expression in stroma fibroblasts with survival in pacients. In other words, patients with a high VDR expression in tumour stroma fibroblasts show better overall survival than patients where VDR expression is lower. This correlation is independent from VDR contents in tumour cells. Thus, vitamin D or its derivatives, which activate VDR in patients whose tumour cells do not express VDR, may have protective effects against colorectal cancer. This is, the stimulation of VDR expression in fibroblasts near the tumour may contribute to a positive evolution of the disease.
All things considered, the results obtained in this study support the convenience of maintaining suitable vitamin D levels, avoiding the decrease occurred in winter, when our skin is incapable of producing enough vitamin D due to low sunlight exposure.
References
- Gemma Ferrer-Mayorga et al (2017) Vitamin D receptor expression and associated gene signature in tumour stromal fibroblasts predict clinical outcome in colorectal cancer Gut doi: 10.1136/gutjnl-2015-310977 ↩
2 comments
[…] Read the complete article… […]
[…] *Imagen de portada: Invasión tumoral de una vena en cáncer colorrectal (Wikimedia Commons). *El artículo completo en inglés está disponible en Mapping Ignorance. […]