Contact lenses to monitor glucose levels: A sweet solution for diabetic patients?

Diabetes is becoming a huge problem in our society, affecting nowadays one in every 20 people in this planet. Although some people don’t know, diabetes is a very serious disease that can cause damage in the heart, blood vessels, eyes, kidneys and nerves, producing different neuropathies, kidney failures, blindness and increasing in the risk of heart disease and stroke, most common death causes of diabetic patients. Not surprisingly, The World Health Organization estimates that 1.5 million deaths in 2012 were directly caused by diabetes and predicts that this disease will be the 7th leading cause of death in 2030 1.
Diabetes is a chronic disease that occurs mainly when a) insulin is not properly produced by the pancreas or when b) insulin is not effectively interpreted/used in our bodies (i.e., the body ignores existing insulin). Insulin is a hormone that regulates blood sugar levels helping to keep them from getting too high (hyperglycemia) or too low (hypoglycemia). That might sound not very important but, unfortunately, the lack of insulin’s function leads to uncontrolled blood sugar levels that over time can cause serious damages in the body. Even more, big and fast unregulated changes in blood glucose (dangerously high or low) can sometimes induce coma states. Thus, controlling blood glucose levels in diabetic patients is really important… but it is not easy.
Some diabetics say that managing blood glucose levels can be like having a part-time job. Glucose levels change significantly with normal activity like eating or exercising, producing peaks and troughs on blood sugar content. For healthy people that is not a problem since insulin is produced and released to regulate availability/usability of glucose – if for example you have more sugar than you need, insulin helps to store it in your liver, which can release it when your blood glucose level is low (i.e., between meals or during exercise). But for a diabetic without insulin properly working, glucose is not that well regulated and therefore its changes can be harmful and have to be monitored and controlled carefully by physicians. Nowadays, glucose monitoring is performed using devices that measure glucose in blood drops. That implicates that all people with diabetes must prick their finger and test drops of blood throughout the day. We all can imagine that this is quite uncomfortable and in fact many people with diabetes check their blood glucose less often than they should, risking their health.
Over the years, scientists have investigated other body fluids in humans trying to find a new, easy and less-invasive way to measure glucose daily. So far, best candidates seem to be tears, airway mucus, sweat, saliva or the interstitial fluid of subcutaneous tissue 2. The last seems to be the more reliable but needs surgery to implant the glucose sensor under the skin. Sweat is not always present and some controversy has been shown for mucus and saliva as reliable readouts for monitoring glucose. Although not perfect, tears and eye fluids might offer a nice and easy alternative readout of blood glucose. But how can we collect tears? How can we measure glucose easily in our eyes? Those were the questions that Dr. Babak Parviz was asking himself. And he came with a cool idea: what if we are able to incorporate glucose sensors in contact lenses and the patient just has to wear them and forget about monitoring blood sugar?
That is the start of the awesome project of developing smart contact lenses, initiated when Dr. Parviz was a professor of University of Washington, Seattle. After that, he joined Google’s experimental X Lab, one of the latest crazy adventures of Google that started in 2010. Google X, normally written as Google[x], is a semi-secret facility based in Mountain View, California, dedicated to scientific research that explores and tries to develop groundbreaking technological advancements for society. A few nice examples of what they are trying to do are self-driving cars, tremor-cancelling spoons for Parkinson’s patients or the world famous google glasses. Not surprisingly, Parviz’s smart lens project fitted perfectly into what Google[x] was looking for and the project was seriously started with the help of Brian Otis and was announced this January, 2014. Since then, the project has been looking for expert biomedical partners to ensure its success, finally announcing this July, 2014 a partnership with the giant European drug maker Novartis 34.
Now the question is: How can they create contact lenses for measuring glucose? This is a very difficult challenge that has to face six main problems: 1) the device inside the lens has to be small enough to not interfere with vision, 2) it should not cause eye irritation, which alters the concentrations of metabolites and proteins within the tear fluid, 3) it has to provide a specific response to glucose and not sense any of the other thousands of metabolites present in tears, 4) it must be designed to not alter contact lens properties (curvature, transparency, softness, etc…), 5) it needs to transmit collected information wirelessly and 6) it needs independent power to work 5.
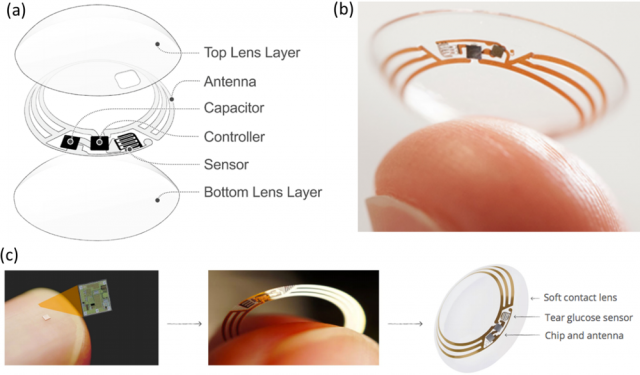
It basically sounds impossible, but Otis and Parviz were able to solve most of the problems thanks to recent advances in electronics, microfabrication techniques, materials and glucose sensing technologies. The design of the prototype is based on a miniaturized electrochemical glucose sensor placed between two layers of hydrogel matrix, the typical contact lens material. The sensor is connected to a tiny battery and a tiny wireless chip that are mounted onto an electronic ring that avoids the iris and pupil. A small pin-hole in the lens allows tears to seep into the sensor, generating blood glucose readings that can be transmitted to a smartphone device using an antenna and the technology known as RFID. This spectacular prototype is able to measure glucose concentration in tears once per second!
Now the team at Google[x] is working to improve these devices. One interesting upgrade is the addition of micro LEDs, which would be connected to the rest of the circuit, and when glucose levels are too high or too low they would be turned on coloring the vision of the patient. That would be a warning signal that tells the patient to correct his/her glucose levels immediately helping to manage the disease in real time and preventing harmful situations such as diabetic comas.
Potentially, these types of contact lens devices could be used for managing/diagnosing other diseases by just changing the type of sensor inside the lens. For example, it has been proposed that monitoring urea in tears could help to detect failures in renal function 6 or measuring dopamine in eye fluids could help to detect early stages of glaucoma 7. In addition, contact lenses can be used for medication delivery and scientists at the Massachusetts General Hospital in Boston have developed prototypes for a lens that releases anti-inflammatory drugs over as long as 30 days.
It is still early days for this lens-based healthcare technology. However, its potential seems enormous. The use of contact lenses is really extended in our society and the number of lens users worldwide has been increasing, standing now at over 71 million. This worldwide use makes these devices very user-friendly and can facilitate a lot the treatment of diseases that require minimal invasiveness and continuous monitoring, such as diabetes. In his own words Dr. Babak Parviz’s says “we hope this [technology] could someday lead to a new way for people with diabetes to manage their disease”. And I think we all hope he is right.
References
- World Health Organization (2014). Diabetes. Fact Sheet number 312. ↩
- Mitsubayashi, K. (2014) Novel biosensing devices for medical applications. Soft contact-lens sensors for monitoring tear sugar. Simulation of Semiconductor Processes and Devices (SISPAD), 2014 International Conference, pp.349,352. doi: 10.1109/SISPAD.2014.6931635 ↩
- Novartis International AG, press release (2014). Novartis to license Google “smart lens” technology. ↩
- Senior, M. (2014). Novartis signs up for Google smart lens. Nature biotechnology, 32(9), 856-856. doi:10.1038/nbt0914-856 ↩
- Farandos, NM, Yetisen, AK, Monteiro, MJ, Lowe, CR and Yun, SH (2014). Contact Lens Sensors in Ocular Diagnostics. Adv. Healthcare Mater. doi:10.1002/adhm.201400504 ↩
- Farkas, Á, Vámos, R, Bajor, T, Müllner, N, Lázár, Á, & Hrabá, A. (2003). Utilization of lacrimal urea assay in the monitoring of hemodialysis: conditions, limitations and lacrimal arginase characterization. Experimental eye research. 76(2), 183-192. doi:10.1016/S0014-4835(02)00276-2 ↩
- Andoralov, V, Shleev, S, Arnebrant, T, & Ruzgas, T. (2013). Flexible micro (bio)sensors for quantitative analysis of bioanalytes in a nanovolume of human lachrymal liquid. Analytical and bioanalytical chemistry. 405(11), 3871-3879. doi:10.1007/s00216-013-6756-x ↩
3 comments
[…] Iaz, 2014. urtean, iragarritako aurrerapen teknologikoa izan zen, etengabe glukosa maila neurtzen duten lentillena. Hau, printzipioz, oso baliagarria litzateke diabetikoentzat… Seguru? Jaime de Juanen artikuluan: Contact lenses to monitor glucose levels: A sweet solution for diabetic patients? […]
were i found the contact lenses to monitor the glucose level,
I live in Pakistan.
available in United Arab Emirates ?
A podiatrist can help you take care of your feet and foot ulcers. A podiatrist will diagnose your diabetes and prescribe the necessary treatments. A podiatrist can also provide treatments for foot ulcers, including surgery if necessary.