At the edge of the cliff: no new antibiotics for multidrug-resistant bacteria
At the edge of the cliff: no new antibiotics for multidrug-resistant bacteria
The Ebola outbreak has brought the fear of a viral pandemic to the headlines once more, as it happened before with the avian or swine flu. Although viruses-caused infections catch most of attention on the media, the greatest risk to human health comes from other microorganisms, the antibiotic-resistant bacteria. Contrary to viral outbreaks, the threat of multidrug-resistant bacteria to human health is a slowly but steadily developing process, a time bomb. The infectious diseases caused by these microorganisms are becoming increasingly difficult to treat, as epitomized by the growing number of acronyms: MRSA, which stands for Methicillin-resistant Staphylococcus aureus, is probably the best know, but the list is long and is increasing: MDR-TB (Multidrug-resistant tuberculosis,) VRE (Vancomycin-resistant Enterococcus), MRAB (Multidrug-resistant A. baumannii) etc. The sub-populations that are not killed by these antibiotics need to be treated with second or third line antibiotics, less effective and often less safe. Alarmingly, due to the lack of new antibiotics we may soon witness multidrug-resistant bacteria strains that cannot be killed by any antibiotic.12
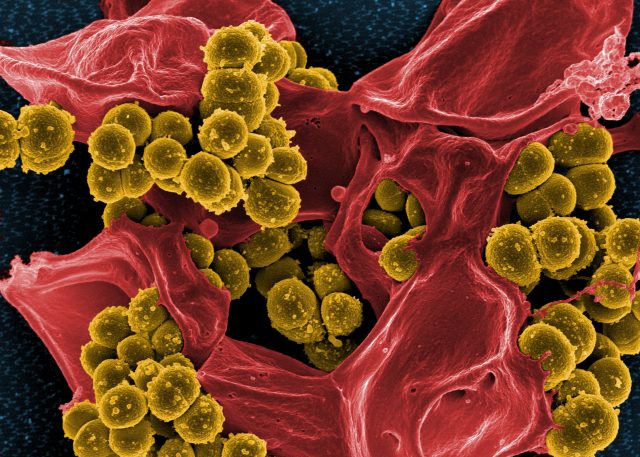
Antibiotics are one of the most effective and commonly used therapeutic agents to protect human live, but every time they are used selective evolutionary pressure is created on the bacteria they target. If any bacteria survive, they are then able to pass on those genetic mutations that conferred them resistance. That is the reason behind being advised by doctors to fully complete the antibacterial treatment even if we start to feel better before. But this is not always the case, and moreover, the global misuse of antibiotics is extended much further: Antibiotics given to treat viral infections is still a common practice in many countries. Not only does not cure the disease, it enhances the chance of later acquiring an antibacterial infection. This nonsense is turn into negligence in cases where massive amounts of antibiotics are poured into the environment from manufacture factories. As an example, one study found the equivalent of 45,000 doses of the antibiotic ciprofloxacin leaking daily to a river. In addition, antibiotics are widely used in livestock and fish farming as growth promoters. As a consequence, resistance rates are increasing worldwide and new mechanisms of resistance are emerging.
Until recently, new antibiotics have been developed to replace ineffective ones. However, we are now in a situation where there are not enough new antibiotics to replace the current arsenal, which is losing efficacy. As major pharmaceutical companies have abandoned antibacterial research and development the pipeline for new antibiotics has been steadily drying out (Figure 2).

Moreover, the antibiotics that are being used currently are the result of scientific discoveries that happened decades ago: There have not been successful discoveries of new classes of antibiotics since 1987.

This figure illustrates well the history of the antibiotics. Although the antibiotic era is often (as in the figure) reported to start with Fleming’s groundbreaking discovery of penicillin in 1928, the first antibiotics go back to the first decade of the century. It was in 1909 when the first antibacterial drug, Salvarsan, was discovered, which was used against syphilis. The first antibiotics, organoarsenicalls and sulfa drugs, were fully synthetic, this is, produced in the laboratory. Fleming´s discovery changed the focus to nature, specifically to fungi. He observed that a substance produced by Penicillium chrysogenum exhibited antibacterial activity, which he called penicillin. However, it was only by the pressure of World War II, several years later, that investment flowed to investigate and develop penicillin as a drug. Both chemical synthesis in the laboratory and fermentation from fungi were attempted. The first failed and penicillin was produced growing fungi in huge tanks. In the following years, a myriad of new complex molecules derived from nature were discovered: streptomycin, tetracycline and erithromicin to name but a few.
These powerful molecules produced by fungi enabled to treat many diseases but they had some drawbacks too. Their chemical transformation upon obtaining the antibiotics from fermentation enabled higher efficacy, safety and bioabailability. This combination of fermentation and chemical synthesis is known as semisynthesis and opened the golden age of antibiotics, back in the 1960’s. It was in this context when the U.S. Surgeon General stated “time to close the book on infectious diseases, declare the war against pestilence won, and shift national resources to such chronic problems as cancer and heart disease”. This was obviously not the case. Bacteria, that have been living in the earth for 109 years responded to the aggression developing mechanisms to avoid antibiotics. As pointed out before, each dose of antibiotics has a double effect: It kills bacteria, but those that survive can pass on the genetic mutations that enabled them to do so. So, the paradox of antibiotics is that we are somehow selecting the most dangerous and resistant bacteria.
However, this has always been the case, and so far we have managed to find new antibiotics. The research and development of a new drug is known to be an extremely costly process for which pharmaceutical companies expect to recover their investment. Nevertheless, with antibiotics this is usually not the case, as they are administered only for short periods. In contrast, drugs to treat chronic illnesses (such as hypertension and diabetes) or cancer offer a greater potential return on investment. Moreover, in the case of antibiotics, the new ones are not used immediately but are kept as the last option, when the others have proven to be ineffective. Although sensible from a medical point of view, it means that the company which developed it has fewer years of exclusive marketing till the patent expires, and therefore, less sales. In summary, pharmaceutical industry does not profit from antibiotic commercialization, and therefore research and development has been steadily abandoned.
Academia-based research is impotent by itself to shoulder the discovery of new antibiotics and small biopharmaceutical companies, currently the motor of the little new antibacterial development, often face difficulties due to the high cost derived from clinical trials. Clearly the problem is more economic than scientific. Several strategies have been proposed to tackle it: public-private partnership, incentives for antibiotic development, philanthropy etc. but all converge in a point: greater investment. It is indeed a required if we want the arsenal of antibiotics to be replenished. Otherwise we might go back the pre-antibiotic era, when catching pneumonia almost inevitably led to death.
References
- Wright P.M. & Andrew G. Myers (2014). The Evolving Role of Chemical Synthesis in Antibacterial Drug Discovery, Angewandte Chemie International Edition, 53 (34) 8840-8869. DOI: http://dx.doi.org/10.1002/anie.201310843 ↩
- World Economic Forum, Global Risks Report 2013. (accessed October, 2014). ↩
2 comments
[…] Pero para qué queremos vivir más y más sanos si después cogemos una infección para la que no tenemos un fármaco que nos cure. Esta es la alarmante situación a la que estamos llegando con los antibióticos y la […]
[…] Baina zertarako nahi dugu gehiago bizi eta osasuntsuago, infekzio bat harrapatuz gero ez baldin badugu sendatzen gaituen botikarik? Egoera honetara heldu gara antibiotikoekin ez baitago mikroorganismoen andui gogorrei aurre egingo dionik. Pablo Ortizen azaltzen digu: At the edge of […]