The “bad luck” of cancer

Trying to know the cause/s of cancer is nowadays a key issue for our society. Scientists and doctors from all over the world are working to study how cancer appears and what factors can increase its risk to help developing new ways of prevention and treatment. Accordingly, government and charity budgets dedicated to cancer research in EU and US are quite significant compared to other areas of research. Just to give an idea, 2014’s budget for the National Cancer Institute (the principal agency for cancer research in the US) was approximately $5.1 billion.
So, what do we know about the cause of cancer? It is becoming clearer that cancer arises from one single cell that it is transformed into a tumor cell with new uncontrolled growing capacities. This new tumor cell is able to divide quickly, creating a mass of abnormal cells that grow beyond their usual boundaries which could invade adjoining parts of the body and spread to other organs in a process called metastasis. This transformation from a normal cell into a tumor cell is a multistage process that involves the acquirement of new “bad” genetic mutations and epigenetic changes (in other words, DNA damage). When a normal cell gets its DNA damaged, it has to decide if it repairs the mutation or if it kills itself in a process called apoptosis. Unfortunately, in a cancer cell, damaged DNA is not repaired neither the cell kills itself. Instead, the cell continues dividing and making new cells which all have the same damaged DNA as the first abnormal cell does. This process is repeated several times and the tumor cell acquires more random mutations that can lead to more growing and aggressiveness of the tumor.
This damage in DNA can be caused by environmental factors, such as physical carcinogens (ultraviolet radiation), chemical carcinogens (components of tobacco smoke, aflatoxin or arsenic) and biological carcinogens (infections from certain viruses or bacteria). It can also be caused by several “internal” (endogenous) factors such as the presence of reactive oxygen species (ROS), metal ions or some metabolic reactions that occur inside the cell. In addition, lots of mutations come from “mistakes” made by the cell during normal cellular division. Before one cell divides in two, it has to copy and duplicate its entire DNA. When the new copy is ready, each of the two daughter cells take one of the copies (simplifying, one takes the old and the other takes the new). Since human genome contains more than 3 billion base pairs (characters or letters that encode genetic information), it is expectable that some mistakes are made during copying. Luckily, the cell also has a repairing mechanism that detects DNA abnormalities and fixes them before the cell divides in two. However, the repairing mechanism can also fail sometimes and when that happens, the mistake (mutation) becomes part of the daughter cell and will be transmitted in the following divisions.
Knowing possible sources of new mutations is important, but what we really need to know is which ones are being nowadays the key factors causing cancer in the population to create prevention strategies accordingly. In addition, knowing the principal sources of new mutations could help to understand why some tissues give rise to cancer in humans a million times more frequently than others (the lifetime risk of being diagnosed with cancer is for example 4.82% for large intestine compared to 0.003% for pelvic bone). Working on this last question, Cristian Tomasetti (a mathematician who studies oncology at the Johns Hopkins University School of Medicine) and Bert Vogelstein (a renowned cancer geneticist at the Johns Hopkins’ Sidney Kimmel Cancer Center) used biostatistics to solve where the differences can come from 1. They plotted for 31 different tissue types the probability of cancer diagnosis during lifetime versus the total number of stem cell divisions in each tissue and found a strong positive correlation between both factors. This correlation could explain that about 65 percent of the variation in cancer risk among different tissues can be explained by the number of stem cell divisions a tissue undergoes within its lifetime. In other words, the bigger the cumulative number of stem cell divisions, the higher the cancer rate in that particular tissue (just as a reminder, stem cells are those that can self-renew and are responsible for the development and maintenance of the tissue’s architecture because the can create any cellular type, from muscle cells to neurons).
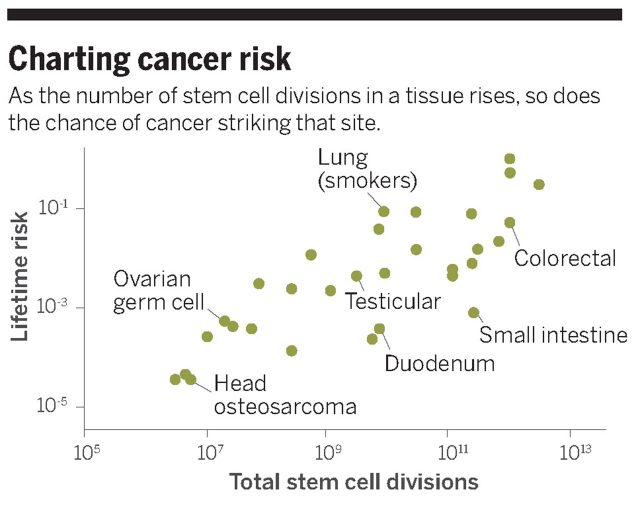
Where is this correlation coming from? How the number of stem cell divisions can affect cancer lifetime risk of a tissue? The answer is directly related to what is explained before. To clarify it, let’s say a particular cell does not divide at all. That virtual cell could have any cancer-related mutations you could imagine but would never develop a tumor since it is not able to divide and transmit its wrong information (DNA damage) to its daughter cells to create a mass of mutated cells (risk of creating a tumor would be 0). Now let’s imagine a healthy cell that divides a lot (as a regular stem cell would do). That healthy cell has to copy its 3 billion DNA characters every time it divides, having each time a small chance of getting a new mutation due to a failure on copying/repairing mechanisms. Therefore one can expect that the more a cell divides, the bigger the chance of getting a cancer-related mutation, and also, the bigger number of highly-dividing cells in a tissue, the greater the chance of getting a mutation in one of those that can cause cancer in that organ.
Taking a look into the correlation shown by the authors, that seems to be true. The correlation is maintained through cancers with enormous differences in incidence and it is extended across five orders of magnitude, pointing out that mistakes during stem cell division can explain the variation in cancer risk among tissues. It also suggests that the “bad luck” of making a mistake during DNA replication can be a major cause for developing cancer although it is of course not the only one. This idea of a “bad luck” component is actually not a new concept and we all know that there is some randomness in developing the disease.
This article has stirred up great interest from newspapers and, very unfortunately, some journalists have understood really wrong the message of the paper, publishing misguided headlines like “Two-thirds of adult cancers largely ‘down to bad luck’ rather than genes” (for example, here) or “Most cancer types ‘just bad luck’” (here). This has made WHO quite angry, prompting them to publish a press release explaining that the major cause of cancer nowadays is not bad luck and that according to current estimates nearly half of all cancer cases worldwide is preventable 2.
What I think it is important to understand here is that the article explains the relative variation in cancer risk among tissues but does not explain the proportion of cancers caused by cell division in our population. So if everybody would smoke 40 cigarettes per day, the correlation found would still be there (more risk in tissues with high stem cell division) but the absolute number of deaths would be much bigger and those deaths would not be caused by “bad luck” but directly by the chemical carcinogens that are components of tobacco smoke. So for our lifestyle the message is the same: please continue using sunscreen, avoiding smoking, eating fruits and vegetables, not being sedentary and not playing with enriched uranium.
References
- Tomasetti C. (2015). Variation in cancer risk among tissues can be explained by the number of stem cell divisions, Science, 347 (6217) 78-81. DOI: http://dx.doi.org/10.1126/science.1260825 ↩
- World Health Organization (2015). Most types of cancer not due to “bad luck”. Press release, N° 231. ↩
2 comments
[…] ¿Qué hay de cierto en esa noticia que ha corrido como la pólvora de que el cáncer es cosa de mala suerte? Pues entre nada y muy poco. Jaime de Juan te lo explica en The “bad luck” of […]
[…] Hara! Zer ote da egiazkoa, bolbora bezain bizi hedatu den, minbizia zorte txarrari zor zaiola dioen berrian? Jaime de Juanek azaltzen digunez, ezer ez edo ezer gutxi: The “bad luck” of cancer. […]