Junk DNA makes you fat
Junk DNA makes you fat
You have around 3,000 million letters in you genome. And so does your neighbour, your boss or your gym instructor. They go like this: ATGC…and so on. The four same letters over and over in endless different combinations. What makes you yourself and, extensively, what makes your boss a distinctive and unique human being, is only a tiny fraction of all the letters in your DNA. You might not like this but you are 99.9% your boss.
But numbers aside, the big question is how these genetic changes make you so different from your boss in your physical appearance, your emotional qualities or your predisposition to suffer diseases. Since DNA contains the recipe to make proteins, even the smallest letter change can modify the sequence of a protein and this might affect its function. For example, haemophilia is caused by small changes in the genome that affect the sequence of a protein involved in blood clotting, making it no longer functional. Unfortunately, the story is not always this simple.
Most of the human genome is considered junk DNA, which does not encode a message to be translated into proteins. Even genes, considered the hereditary units in our genetic information, aren´t continuous stretches but instead they contain large chunks of junk DNA in between the protein-coding regions. When the cellular machinery is reading the message to make proteins, it skips these parts that are known as introns. In principle, introns and all the other DNA parts that aren’t used to make proteins were thought to be a consequence of evolution, but to have no function otherwise. However, some of the DNA that for decades was considered useless is proving not so junk anymore.
Obesity is one of the main epidemics in the western world and big resources are dedicated each year to find possible genetic causes behind this disease. Many studies comparing obese and lean people found changes in 74 different locations of the genome that were associated with obesity. This is normally the case for complex diseases such as cancer or diabetes where there usually are many genetic factors involved. However, this time the surprise came when the strongest association with obesity was found in a junk DNA location. So obese people have differences in DNA letters that don´t affect the sequence of any cellular protein. The question was then: how can these differences be so important to produce huge variations in your body weight?
The answer, as it happens, was not easy to see1. The region linked to obesity was found to be in one of the introns of a gene. And this gene was consequently christened FTO (fat mass and obesity associated gene) for obvious reasons. It was assumed that somehow these letter changes in the intron might make it more difficult for the cellular machinery to read this gene, ultimately decreasing the expression levels of the protein. And since this protein was known to be involved in the metabolism of fat, everything seemed to fit pretty well. The problem was that this could never be proven.
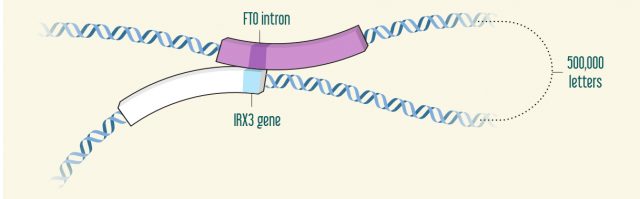
FTO was being held as the main suspect for obesity whereas the real culprit was very far away in the genome. Not less than 500,000 letters away. But the genome it´s not a linear structure; it´s more like a ball of wool. And it turned out that the first intron of the FTO gene was physically interacting with a distant gene and by doing so was actually controlling how much protein was produced from this gene. What was even more interesting was that this same three-dimensional structure was present not only in humans but also in mice and fish. This demonstrated a very important function for this intron throughout the evolution of vertebrates in the regulation of other gene(s). Nothing further from the junk DNA denomination.
The rest of the story that followed was that the gene regulated by the FTO intron, named IRX3, is also a major regulator itself that controls the action of hundreds of genes. Ironically, many functions but the control of body weight had been ascribed to this gene. However, it was soon to be found that mice lacking this gene are much thinner and have much less fat than normal animals. Apparently, this function is carried out in the hypothalamus, a brain region where IRX3 controls food intake and metabolism. In the end, the genetic predisposition to obesity is not only revealing a fabulous biological mechanism but also suggesting that this disease has a major nervous component.
When the human genome was finally sequenced in the beginning of the century, the cure to disease was celebrated (mostly by over-reacting politicians) around the world. Now, ten years down the line the puzzle is looking increasingly difficult to solve. Not only do we have to deal with mechanisms that control the genome without altering its sequence but also with changes in the sequence of supposedly non-functional junk DNA areas that have a major effect on far away genes. Biology has probably always been as intertwined as a ball of wool. The difference is that now we are starting to realise.
References
- Smemo S., Kyoung-Han Kim, Eric R. Gamazon, Noboru J. Sakabe, Carlos Gómez-Marín, Ivy Aneas, Flavia L. Credidio, Débora R. Sobreira, Nora F. Wasserman & Ju Hee Lee & (2014). Obesity-associated variants within FTO form long-range functional connections with IRX3, Nature, 507 (7492) 371-375. DOI: http://dx.doi.org/10.1038/nature13138 ↩
1 comment
is junk DNA really junk?