Living with half a brain
Living with half a brain
Many people think of their brain as a computer full of microchips and wires, as a storehouse full of memories and learned things, as a clock with millions of mechanisms intimately intertwined with each other, so it is incredible to think that someone can live with much less than that, with only one brain hemisphere. And yes, it can happen. It’s rare but there are few dozens of people who live without large parts of their brain, half or even less.
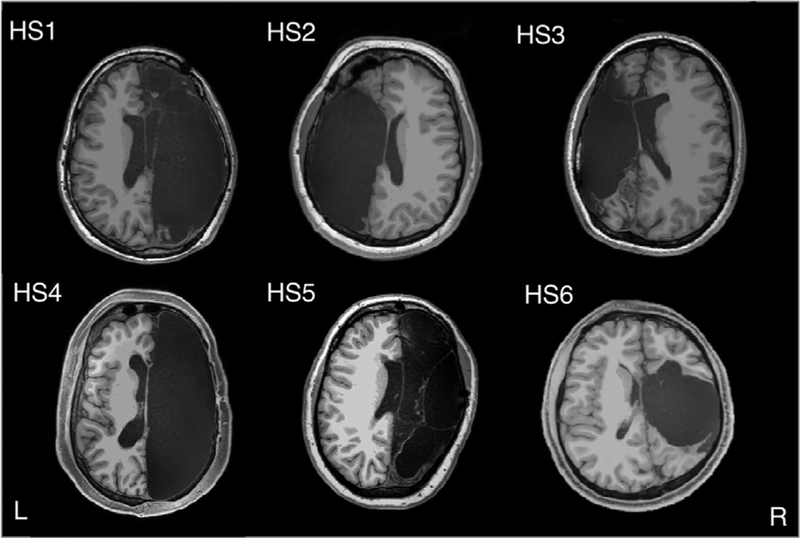
These people weren’t born that way. Most commonly they had a disease in childhood, such as Rasmussen’s encephalitis, where epileptic seizures are very common. We can think of epilepsy as an electrical storm, which is urgent in a particular area of the brain and spreads through the brain as if it were clouds moving forward and releasing lightning. When this train of impulses reaches a particular area, the neurons in that area start firing and the storm continues to spread. Thus, when the wave of electric shocks reaches the area of the brain involved in the movements, the motor cortex, many rapid muscle contractions are produced in different areas of the body and convulsions arise.
There are many epilepsies that respond well to drugs and are perfectly controlled, but there has always been a percentage that are called refractory, which do not respond to treatments, and other diseases where the brain tissue is damaged. Seizures can be so frequent that the child, because in these cases we are talking about children, cannot develop normally because the brain is never at rest, or is having a seizure or is recovering from a seizure. One solution is to destroy the epileptic focus, the starting point, but if it cannot be identified and the brain is damaged by the seizures, another possibility is to remove a large area.
A recent study 1 by Kliemann et al., from November 2019, has analyzed the brains of six people who had this operation, one brain hemisphere had been removed, which is called a hemispherectomy. The results were compared with those of six other healthy adults who also had scans and a database that included the results of 1,500 other healthy adults, with an average age of 22.
The youngest patient was three months old at the time of surgery while the oldest was 11 years old. All six patients had suffered epileptic seizures since they were young children, one of them having had the first seizures within minutes of birth. In four of them the right side of the brain was removed while in the remaining two it was the left side. The causes were varied: in two cases it was a stroke around birth, in three others it was Rasmussen’s encephalitis, which causes epilepsy and brain damage, and in the sixth it was cortical dysplasia.
The six patients volunteered for functional MRI, a technique that allows them to view the functioning brain with good spatial and temporal resolution at the California Institute of Technology (Caltech) Brain Imaging Center in Pasadena. The results were compared with those of six other healthy adults who were also scanned and with a database that included the results of 1,500 other healthy adults, with an average age of 22. What has attracted attention is that these people, who were now in their twenties or thirties, functioned remarkably well, had jobs, their language functions were normal and when they were put on the scanner they chatted as any normal person.
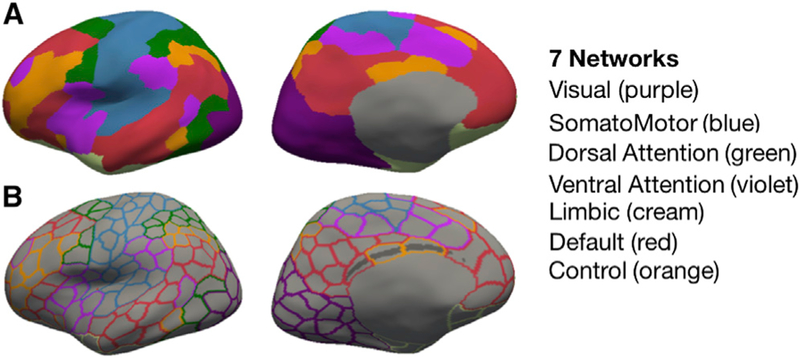
The researchers divided the brain into 400 areas, 200 in each hemisphere, and established seven functional networks. The same pattern of plots seen in healthy people could be easily distinguished in people with half a brain. The second phase was to see if the same person was scanned again after a while and in the same person and for the same task the same pattern of activity was seen, which is known as fingerprinting. The result of this second part of the study is that the activity patterns were consistent over time. That was the basis for the final study, to see if the functional networks of participants with half a brain were the same or different from those of healthy people.
In the brain there are a series of neural networks, of functional circuits that are believed to be the substratum of our emotions, of cognition, of behavior. The researchers looked especially at brain activity in the networks that regulate vision, movement, emotions and thought, the so-called cognitive processes. Since neural networks dedicated to a single regulatory function often extend across both hemispheres, the research team expected to see weaker neural activity in hemispherectomy patients, but this was not the case. The group of scientists was able to recognize the same networks in the patients with hemispherectomy and the main and surprising conclusion was that the six operated people and the controls showed a powerful and similar connections between the regions the brain regions that are typically assigned to the same functional network. However, the connectivity between regions of several different networks was much greater in all participants who had had a hemisphere removed and between all networks than in the control individuals. These controls were similar for intelligence level, age, hand preference, i.e., whether they were left-handed or right-handed, and gender.
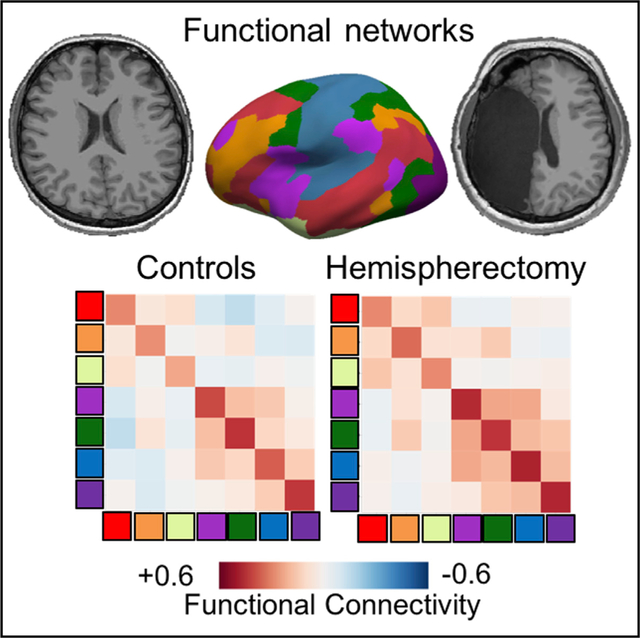
The doctors had already seen that the patients with hemispherectomy functioned at an excellent level but what attracted most attention was the high degree of compensation seen in the neuroimaging study. All of them, even those who had had their left hemisphere removed, where most people’s speech-related areas such as Broca’s or Wernicke’s area are located, were able to speak. It appears that the speech area is shifted from one hemisphere to another after the surgery. If the left hemisphere is missing or damaged, the speech area is located in the right hemisphere. These results support the hypothesis that a shared system of functional networks makes cognition possible and suggests that interactions between different networks may be a key aspect of functional reorganization after a hemispherectomy.
These results were unexpected and interesting because much smaller lesions produced by a stroke, an accident, a tumor or other reasons cause devastating effects. This great capacity for recovery is probably based on two aspects: the brain has many redundant systems and, perhaps more strikingly, it has an enormous capacity for adaptation and flexibility, which is called neuronal plasticity. It would therefore be important to understand how the brain sets these restorative or compensatory processes in motion, in order to implement strategies that improve the prospects of these treatments.
References
- Kliemann D, Adolphs R, Tyszka JM, Fischl B, Yeo BTT, Nair R, Dubois J, Paul LK (2019) Intrinsic Functional Connectivity of the Brain in Adults with a Single Cerebral Hemisphere. Cell Rep 29(8): 2398-2407. doi 10.1016/j.celrep.2019.10.067 ↩
5 comments
[…] Garun erdiarekin bizi daiteke? Eta erdiarekin baino gutxiagorekin? Baiezkoa da erantzuna, baina, zelan? J.R. Alonsoren Living with half a brain […]
Amazing!!
[…] This is supported by the fact that there are people living and functioning with only one brain hemisphere. It appears that the brain is very adaptable. For instance, the speech area shifted from the left to the right hemisphere […]
[…] Living with half a brain […]
[…] It’s rare but there are a few dozen people who live without much of their brain, half or even less. These people were not born that way. The most common is that they have had a disease in childhood […]